Syndromic testing: A powerful approach for simultaneous pathogen detection
Find out how to rapidly test for multiple disease-causing microorganisms with syndromic panel-based testing
12 Oct 2020
The traditional diagnosis of a bacterial, viral, fungal, or parasitic infection can involve a lot of guesswork. Some tests can be insensitive, and most are only able to detect one pathogen at a time, leading to several questions for the physician: Which organism should be tested for first? Should it be the most common cause? Should it be the most lethal cause? Or should it be the most treatable cause?
A syndrome is a set of signs (features apparent to the patient) and symptoms (measurable indications of disease) that characteristically occur together.
In the wake of the COVID-19 pandemic, clinicians are looking for innovative diagnostic techniques to more quickly identify the specific pathogens causing patient illness. Syndromic testing is a powerful approach whereby multiple pathogens, that could be causing the reported signs and symptoms, can be tested for in a single test. Using this approach, providers can order tests for a variety of syndromes based on the patient’s symptoms that can return actionable results faster than traditional testing.
Syndromic testing case example
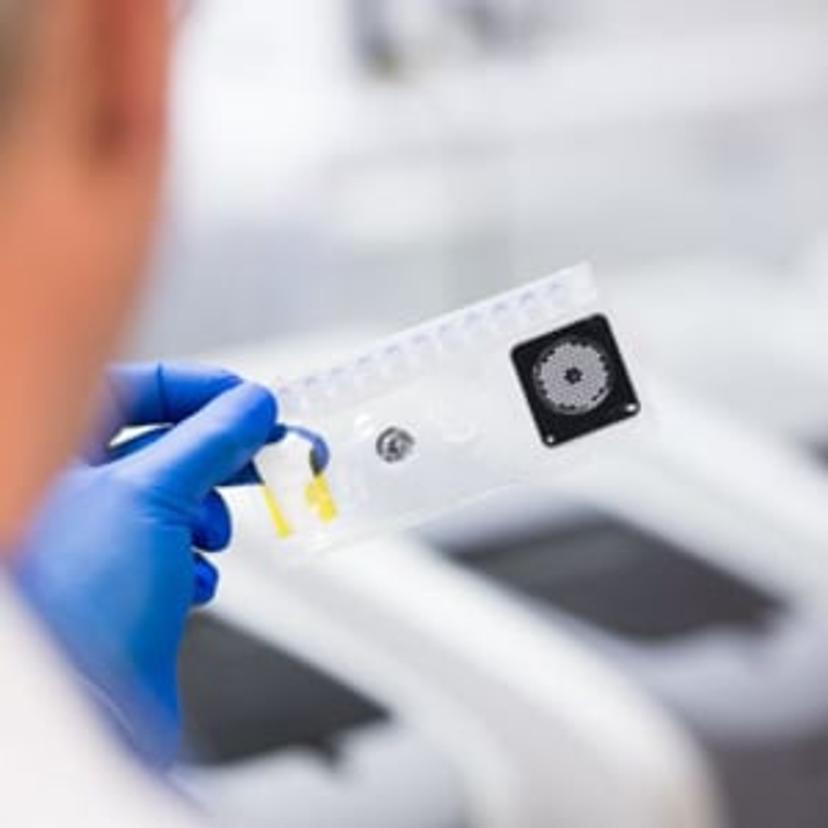
If a patient enters a physician's office with respiratory symptoms, there are multiple organisms that could potentially be the cause of this and being able to identify what organism it is can improve the treatment plan for the patient. Traditional testing is only able to test for a small number of organisms, like influenza and respiratory syncytial virus (RSV), but many other organisms can cause common respiratory symptoms. This means if the physician only tests for influenza and the patient actually has rhinovirus, one of the most common respiratory pathogens, then the result will come back negative and additional testing may still be needed to find the culprit. Respiratory symptoms are predominantly caused by viral pathogens and being able to identify which virus it is can help the physician to avoid potentially unnecessary antibiotic prescriptions.
With a comprehensive respiratory syndromic test, the physician would be able to see that the patient is negative for flu, but positive for rhinovirus. At that point, the physician can create a better-informed treatment plan and avoid the guesswork that comes with not knowing what pathogen is causing symptoms. Syndromic testing increases the probability that a clinician will find out what is making a patient sick, in a shorter timeframe, with a single sample, which improves patient care.
How to conduct syndromic testing
The BioFire® FilmArray® System is designed to provide rapid and accurate syndromic testing via multiplexed polymerase chain reaction (PCR) technology. This process simultaneously isolates, amplifies, and detects the genetic material of an extensive range of microorganisms that could be causing the patient’s syndrome.
“If you want to know what's making your patients sick, choose syndromic testing,” states Wade Stevenson of BioFire Diagnostics. “Our tests are designed to give clinicians the best chance of finding out what is likely making patients ill.”
BioFire now has several different syndromic panels on the market. These comprehensive panels are designed to increase the probability of identifying the most likely cause of different symptoms by combining testing for a broad group of probable pathogens into a single panel.
- BioFire® Respiratory 2.1 Panel (EUA)*>>
Test for the usual respiratory suspects, including Influenza and SARS-CoV-2*. - BioFire® FilmArray® Pneumonia Panel >>
Help distinguish between colonizing and infection-causing bacteria with semi-quantitative results and promote antimicrobial stewardship. - BioFire® FilmArray® Meningitis/Encephalitis Panel >>
Distinguish between bacterial and viral meningitis and optimize life-saving therapy. - BioFire® FilmArray® Gastrointestinal Panel >>
Test for the most common pathogens associated with gastroenteritis. - BioFire® Blood Culture Identification 2 Panel >>
Test for a broad group of pathogens and antimicrobial resistance markers to help improve the management of patients with bloodstream infections.

If you want to know what's making your patients sick, choose syndromic testing.
Wade Stevenson BioFire Diagnostics
Diagnostics for new disease states
Viruses and bacteria are known to evolve much quicker than any other organism on our planet. As a result, BioFire must constantly monitor trends to make sure that its assays continue to be relevant to the current circulating pathogen strains. In addition, new pathogens can sometimes pop up rather unpredictably, such as the novel SARS-CoV-2 virus that causes COVID-19. In such cases, BioFire has to react quickly to enable its panels to detect these new targets and new pathogens. “When SARS-CoV-2 hit, we knew it was important to add the ability to detect this virus to our respiratory panel, and were able to do so in less than 60 days,” Stevenson explains.
BioFire is continually improving its existing panels and exploring new potential disease states to bring to the market. With input from its customers, its in-house scientists, and its sales and marketing teams, BioFire continues to push the technology. Whether or not the concept is deemed feasible is dependent on whether or not it meets BioFire’s core criteria: is it faster; is it cheaper; and is it more effective?
“The next disease state that we're going be moving into is bone and joint infections,” shares Stevenson. “Whether the joint is infected, or there is a mechanical problem with a patient’s prostheses, we want to be able to quickly identify probable infectious causes and advise orthopedic surgeons accordingly.”
There are also opportunities for expansion beyond testing for pathogen DNA. “Traditionally our tests directly identify pathogens based on the presence or absence of their DNA,” Stevenson explains. “However, we can now identify the presence of a pathogen by monitoring the body's response because your body activates unique sets of genes depending on whether the infection is bacterial, viral, fungal, or something else entirely, like an autoimmune response.” The access to screening capabilities that can rapidly and accurately differentiate these responses is a critical tool in the clinic that may help avoid the unnecessary use of antibiotics, reduce the length of hospital stays, and ensure effective patient care.
Learn more about syndromic testing from BioFire here >>
*About Emergency Use Authorization:
• This test has not been FDA cleared or approved.
• This test has been authorized by FDA under an EUA for use by authorized laboratories.
• This test has been authorized only for the detection and differentiation of nucleic acid of SARS-CoV-2 from multiple respiratory viral and bacterial organisms.
• This test is only authorized for the duration of the declaration that circumstances exist justifying the authorization of emergency use of in vitro diagnostics tests for detection and/or diagnosis of COVID-19 under Section 564(b)(1) of the Act, 21 U.S.C. § 360bbb-3(b)(1), unless the authorization is terminated or revoked sooner