Organ-on-a-chip provides preclinical safety toxicologists with the tools to combat drug attrition
Learn how organ-on-a-chip technology is aiding toxicologists in de-risking drug-induced liver injury by providing human-specific safety data
16 Oct 2023

The liver is responsible for metabolizing most medications, and as such represents one of the primary tissues susceptible to drug-induced injuries. Drug-induce liver injury (DILI) represents a major cause of drug attrition within the preclinical stages of drug development and clinical trials, plus, more than 750 FDA-approved drugs are flagged for some degree of DILI risk1. To combat high attrition rates, DILI in humans needs to be identified earlier in the preclinical discovery pipeline.
Traditionally, in vitro experiments using proliferative cell lines and animal models have been adopted to assess the safety of a new therapeutic compound. These approaches have several constraints including limited relevance to humans and a history of falsely identifying toxic drugs as safe. In this SelectScience® interview, Dr. Tomasz Kostrzewski, VP Science & Technology at CN Bio, discusses how organ-on-a-chip technology can help overcome these challenges by providing human-specific safety data.
The need for human-relevant, translatable data
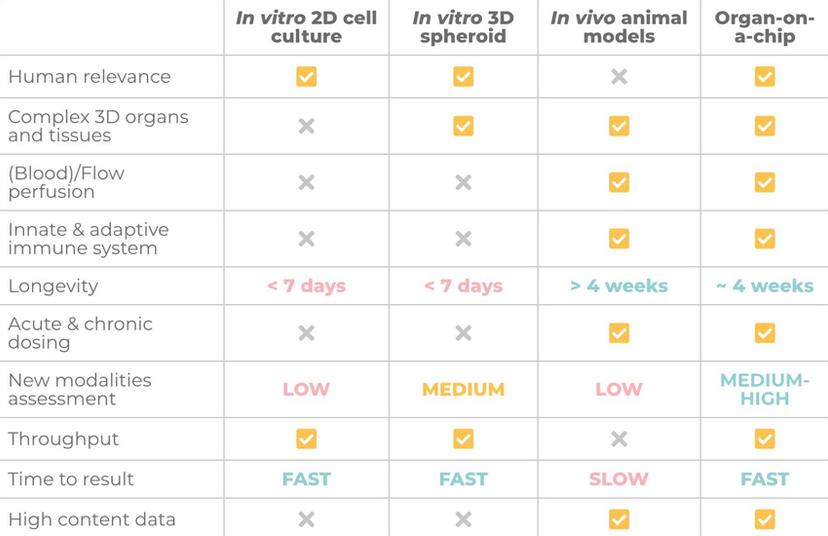
“The challenge that preclinical safety toxicologists are facing is that animal models and simplistic 2D cell-line-based assays can’t accurately predict what happens in a human patient” explains Dr. Tomasz Kostrzewski. “General in vitro assays aren't physiologically relevant enough and are not able to incorporate an immune element. With the increased interest in immune modulatory molecules as potential therapeutics, there is a requirement for preclinical assays to have an immune component. You need to be able to understand whether your drug is going to treat the disease or whether it's going to cause off-target effects in a human-specific preclinical model.”
Animal models are also poor predictors of drug safety in humans and have a history of falsely identifying toxic drugs as safe and labeling useful drugs as toxic2. “With animal models, we can look at drugs in the system however, different species have very different immune cell types and regulatory pathways to humans. These interspecies differences can pose a risk, should liabilities pass undetected, or a waste if a promising drug is removed from development unnecessarily. Another challenge that preclinical toxicologists face is how to approach the safety testing of new drug modalities. These are very human-specific in their modes of action and therefore render animal models less suited,” says Kostrzewski.
Focus has now turned to advanced, in vitro 3D models to provide the solution and address the gap between standard preclinical models and the human. Kostrzewski continues to discuss CN Bio's experience using in vitro 3D liver models to predict human DILI liabilities in order to facilitate more informed decision making.
Organ-on-a-chip technology brings confidence to drug-induced liver toxicity testing
Organ-on-a-chip technology, also known as microphysiological system (MPS), arose out of the need for more predictive human-relevant in vitro preclinical assays. MPS such as the PhysioMimix™ OOC range of Single- and Multi-Organ systems are bio-engineered microfluidic platforms. They provide a scaffold that allows cells, typically relevant combinations of primary human cells, to form a three-dimensional tissue-like structure. Microfluidics perfuse the tissue with cell culture media. The flow and movement of media supplies nutrients and oxygen to the tissue structures, creating a microenvironment that also provides relevant mechanical cues. The overall benefit of this technology is that you can create a stable, much longer-term in vitro cell culture that better recapitulates human tissues and their functions.
“Organ-on-a-chip gives you the ability to cross-reference and sanity check versus the output of animal models so that you don't get things slipping through to the clinic that should have been identified as toxic or vice versa,” Kostrzewski explains. The approach also gives users the ability to obtain mechanistic insights into a drug and its mode of action. “It is not possible to perform mechanistic studies with traditional in vitro assays due to their simplicity. Species differences can also make recapitulating clinical toxicology difficult. Organ-on-a-chip allows users to perform mechanistic studies that can’t be performed in simple in vitro assays or in animals,” says Kostrzewski.
These systems have been developed as single-organ systems where you model a specific tissue, or as interconnected multi-organ systems i.e., a liver model plus an additional organ, such as the gut or lung. “By recapitulating how organs interact and communicate as part of a complex system and using microfluidics to allow drugs to move between these microtissues, you can mimic ever more closely the type of things that happen in a human,” explains Kostrzewski.
Organ-on-a-chip instrument considerations
Organ-on-a-chip offers the potential to unlock human relevant insights that other technologies could miss. Their adoption to supplement and enrich data sets facilitates more confident decision making. There are a number of different technology types available so what should you consider before investing? Firstly, it is important to ensure you can replicate the tissue structure that you want to mimic and the characteristics that you want to see the microtissues capture.
“Another key consideration when looking at technology is the ability of the system to be adaptable, to be able to customize assays to meet your needs, or to address questions as they arise by adding in more cell types,” continues Kostrzewski who concludes with a thought about data - what do you need to generate and over how long? "If you want to perform longitudinal studies, you need a means of repeatedly removing samples for analysis, or imaging. If you would like to perform high content -omics style analysis to unlock mechanism of action you need a solution that provides high volumes of recoverable media and tissue per experimental condition and, if you want to explore the effects of chronic dosing in vitro, you will need a system that keeps cultures viable for as long as 'humanly' possible! The final consideration relates to the skill set of your team. If there is little to no organ-on-a-chip expertise, make sure you adopt an approach that offers an easy transition from 2D into 3D cell culture. Your vendor should also be able to provide you with a reliable access to primary human cells that are pre-validated for use in complex 3D assays to ensure a smooth path to adoption."
Continuing to meet the needs of the pharmaceutical industry
Using clinically relevant biomarkers, organ-on-a-chip can help provide the in vitro to in vivo translatability required by the pharmaceutical industry to reduce drug attrition. As the industry evolves there will be a focus on several key developments for organ-on-a-chip technology.
Kostrzewski describes the need for ever greater levels of validation and characterization data using translationally relevant endpoints. “You need to be able to detect a wide range of endpoints, not just traditional in vitro ones like lactate dehydrogenase (LDH) release or cellular adenosine triphosphate (ATP) content but key translational biomarkers - e.g., for DILI these would be alanine aminotransferase/ aspartate aminotransferase (ALT/AST) release, albumin production, gamma-glutamyl transferase (GGT) or alkaline phosphatase (ALP) release. These translatable endpoints, enable researchers to more directly correlate preclinical data with clinical data.”
Additionally, the portfolios of drug discovery companies are no longer dominated by small molecules. A wide variety of different therapeutic types are in development from biologics to new drug modalities such as RNA and cellular therapeutics. Testing the safety and efficacy of new therapeutic entities with very specific human modes of action, requires an adjustment to the tools in the preclinical toolbox. Where animals are less suited, our reliance on technologies to help plug the human-relevance gap, such as organ-on-a-chip, becomes ever greater.
Future outlooks for organ-on-a-chip technology
PhysioMimix™ OOC Microphysiological Systems enable users to recreate a test environment that accurately represents the human body so that you can generate clinically-translatable data.
Organ-on-a-chip's ability to improve in vitro assay sensitivity and deliver an alternative human relevant testing environment where animal models are less suited, uniquely positions the technology to predict DILI risk in the early stages of drug development. To continue to improve our understanding of immunological aspects of DILI, CN Bio are building even more immunological components into the tissues that they offer, "We continue to develop our offering" says Kostrzewski. "Many immune components have been incorporated into our liver model already such as liver-specific Kupffer cells. Customers of ours have presented work at conferences where circulating T cells or mixed immune populations (e.g., peripheral blood mononuclear cells (PBMCs)) have also been incorporated into the fluidic flow that perfuses tissues too. We intend to develop an ever-wider array of liver models capturing ever greater levels of immune complexity".
The quality of the primary human cells that go into these systems are essential. “The use of pre-validated cells that have been prechecked to ensure they consistently form the same three-dimensional microtissues and behave at a fairly standard level greatly enhances the reproducibility of your data,” Kostrzewski states, "This is why we enable customers to purchase 3D validated cells from lots that have passed our own stringent QC tests. To meet this demand, we work closely with several partners."
Efforts to improve the accessibility and throughput of existing organ-on-a-chip systems are also likely to form key areas of future development. “We are keen to continue to develop and enhance our ‘in-a-box’ products such as our PhysioMimix™ NASH-in-a-box,” explains Kostrzewski. “These products provide you with the ability to quickly and easily recreate CN Bio validated models in your own laboratory, irrespective of your prior experience. They contain the multi-chip plates required for 3D tissue culture as well as all the reagents, primary human cells, and the protocol." Kits are designed for sole use with CN Bio's PhysioMimix Single-and Multi-organ MPS, where guided software takes the operator on a step-by-step journey from the start to the end of the experiment.
Kostrzewski concludes with an insight into CN Bio’s work on the throughput of their PhysioMimix organ-on-a-chip systems, “Our current solution for modeling the liver is a 12-unit multi-chip plate. Using this plate, you can culture 12 livers per plate, and the system can run up to six of these plates, which gives you a reasonable level of throughput compared to single-chip alternatives. We are now looking at how we can enhance this throughput further. We have just released a new solution, the PhysioMimix Single-organ higher-throughput (HT) System and associated Multi-chip Liver-48 plate. This system miniaturizes the chips to incorporate 48 chips into a particular plate and each system enables multiple plates to be run simultaneously. By significantly increasing the throughput, preclinical toxicologists can now make data driven decisions from predictive human-organ models earlier in the preclinical workflow than ever before.”
Want to know more about this topic?
Learn more about using microphysiological systems for predicting drug-induced liver toxicity, in this application note >>
References
Thakkar S, Chen M, et al. The Liver Toxicity Knowledge Base (LKTB) and drug-induced liver injury (DILI) classification for assessment of the human liver injury. Expert Review of Gastroenterology and Hepatology, (2018) Jan;12(1):31–38. Pubmed
Van Norman, G.A. Limitations of animal studies for predicting toxicity in clinical trials, JACC: Basic to Translational Science, (2020) Apr; 5(4): 387–397. Pubmed




