Hijacking the immune system: Discover how extracellular vesicles can be used as a natural drug delivery system
Virologist Dr. Ryan McNamara discusses viral hijacking of extracellular vesicles and its potential for informing novel biotherapeutics
8 Jul 2020
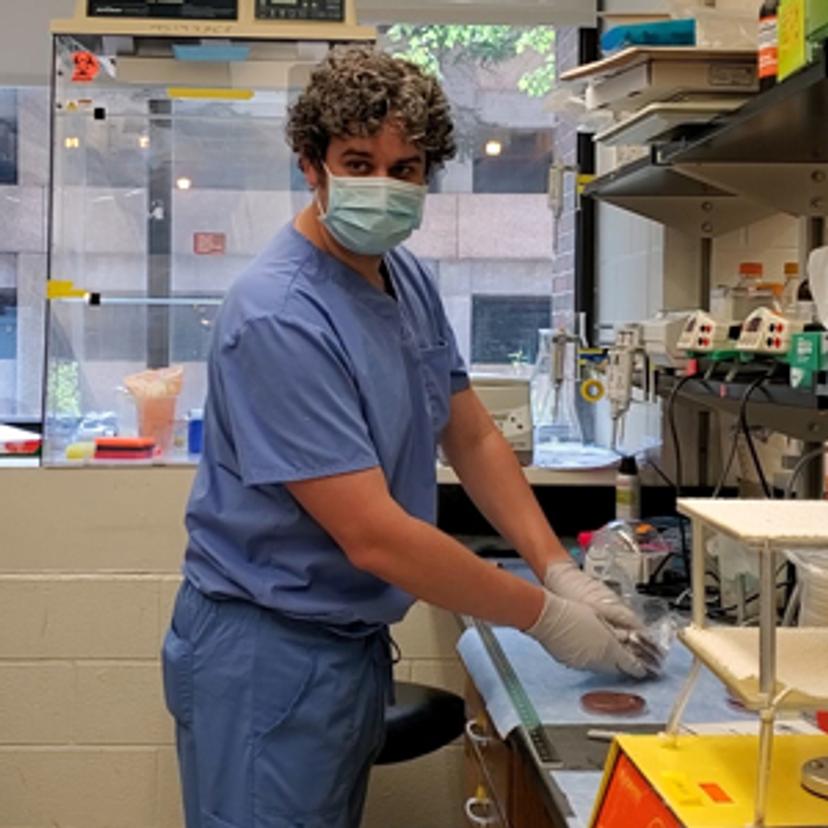
Extracellular vesicles (EVs) are a relatively young field of research generating great interest as a result of their role in intercellular communication. In this SelectScience® interview, we hear from Dr. Ryan McNamara, Translational Fellow at UNC Chapel Hill and Lineberger Comprehensive Cancer Center, about his work on how infectious diseases hijack EVs to facilitate viral spread and why this has implications for multiple areas of science, from cancer research to drug delivery. McNamara discusses current challenges in his research field and the technologies helping to overcome them before looking ahead to future trends in EV use as biotherapeutics.
Tell us about your work on extracellular vesicle function
Extracellular vesicles are released by just about every cell in the human body. It has become apparent in the past two decades that they act as vehicles to transfer material from one cell to the next. I use a virology-based approach to understand how infectious diseases hijack EVs to rewire recipient cell signaling. What we have found is that evolutionarily distinct viruses such as HIV and herpesviruses converge on EV-mediated signaling by incorporating viral elements inside of them. These virus-modified vesicles are then taken up by nearby cells to facilitate in establishing a niche favorable for pathogen takeover. So, viruses can modify cells through EVs without infecting them per se.
How about their potential as biotherapeutic products?
As far as their biotherapeutic potential, I think EVs present several unique advantages. Probably first and foremost is that they act as natural messengers, and our immune systems recognize them as “self” and not foreign bodies like a virus. When your body is exposed to a virus, your immune system moves quickly to stop the initial spread and then develops antibodies towards it to prevent infection in the future. EVs do not elicit this immune response, which is probably why viruses evolved to hijack them to transport viral factors. A second advantage of using them in biotherapeutics is their sheer concentration in biological fluids. They far outnumber even high-titer bloodborne viruses such as HIV and Ebola, and so your body can tolerate them in high doses without going into a shock response. Lastly, it has been shown that the encapsulation of drugs inside artificially produced vesicles can limit their toxicity. One drug that comes to mind is doxorubicin, which is an anti-cancer drug. Treatment with the drug alone in patients results in its accumulation in the heart, and that can have very adverse effects. In contrast, when doxorubicin is incorporated into liposomes, its toxicity and heart-accumulation is decreased. Several groups have investigated how EVs compare and contrast to artificial liposomes in delivering drugs.
What important questions are you looking to answer through this research?
There are several questions that I’m looking at right now in terms of EVs, but they all revolve around how viruses employ them to promote pathogenesis. Viruses can overtake a host despite often encoding only a handful of genes. So, they have had to evolve over the course of many millennia to hijack several distinct cellular signaling pathways. The communication through EVs presents itself as a very stealthy way to transfer materials from a virus-infected cell to a non-infected cell because EVs are recognized as ‘self’ by the immune system. The immediate questions I’m looking to answer are:
How are virus factors trafficked into EVs?
Does a virus alter EV contents differently at different stages of infection?
Since viruses incorporate viral factors into EVs, can we use EVs for liquid biopsy?
And your big-picture goals?
The bigger picture is that we can learn so much about EVs through viruses. It has long been recognized that if a virus is intentionally disrupting a pathway, then it’s almost a certainty that that pathway is very important for normal cellular processes. The study of virus-host interactions has bolstered our knowledge of many aspects of biology such as gene regulation, transport, immune responses, and tumor progression. If we can understand how EVs are modified by viruses to promote disease progression, then we can use that knowledge to understand how tumors are likewise using EVs to promote metastasis. We may think that virus infection and tumor metastasis are very different fields, but the reality is that they can share a lot in common.
What techniques do you use in your lab work to address these questions? How do they help you overcome any challenges in researching extracellular vesicles?
There are several ways to isolate EVs, but I prefer to use methods that allow for large input material to improve product yield. One method to do this is called tangential flow filtration, which can filter and concentrate a solution over time. In our case, we are concentrating EVs from an input fluid while removing other extracellular debris. This technique can be used for tissue culture supernatant or primary fluids such as blood plasma or pleural fluid. This is the first step in concentrating EVs from an input solution.
Viruses and EVs share many biophysical properties such as size and densities. Since a lot of my work focuses on the interplay between viruses and EVs, I must do an extra step to separate them from each other. I use the antibody-based capture of EVs to separate them from virus particles. Other technologies are emerging to address this problem, but for the time being, antibody capture works for me.
How are you using Thermo Scientific™ Nalgene™ Rapid-Flow™ filter units in your work and how have they impacted your workflow?
For more info on the Nalgene™ Rapid-Flow™
Learn how to improve accuracy and consistency in cell culture with the right filtration system: Read the interview
Before putting the input solution into a tangential flow operator, the solution needs to be filtered so that the machine will not clog up. Since we are using large input volumes, often around 1 liter, we need to be able to rapidly filter large volumes of solution. The Rapid Flow filter can accomplish this in a sterile manner, meaning that I can filter my input solution without worrying about contaminating the solution. They can really make the EV workflow go much more quickly and efficiently.
What experimental results have you seen so far?
Thus far, I’ve published three first-author manuscripts using the Rapid Flow filter units for EV isolations (PMID: 30533204, 30716130, and 29437924). The results are consistent across cell lines and primary fluids from different donors. One of the most important aspects of molecular biology is consistency over time and in independent hands.
What do you see for future trends in extracellular vesicle use as biotherapeutics?
There’s so much work going into EVs from so many angles right now. The developing consensus from independent groups throughout the world is that EVs act as vehicles to transport biologically active materials from one cell to another. To that end, there is so much low-hanging fruit in this field for the basic sciences, applied sciences, and medicinal sciences.
I think that characterizing how incorporated contents alter recipient cell physiology is an especially hot area in infectious diseases and cancer biology. Additionally, how we can detect these markers is becoming a field of increased interest. EVs can capture a snapshot of the physiology of the cell it comes from. If the cell is infected with a virus, oftentimes a virus-specific marker can be identified in the EV. If the cell is part of a cancer, tumor-specific markers in EVs coming from it can be identified. Other groups have taken advantage of EVs’ natural function to repurpose them as drug delivery agents. Much of the interest in the field is owed to the ability of EVs to transport materials without activation of the immune system. If we can deliver drugs using natural delivery vehicles, I think that it provides a new approach in the pharmacological sciences.
Learn more about how your choice of filtration device can impact overall performance in this application note, plus visit the SelectScience Biopharmaceuticals Special Feature.
Do you use Thermo Fisher Scientific products in your lab? Write a review today for your chance to win a $400 Amazon gift card>>

