Predictive pharmacology: Novel 3D drug testing systems for improved predictive accuracy
Meet the preclinical contract research organization that specializes in the pharmacology of spheroids
9 Feb 2020
Editorial article

In this article, we interview Dr. Gonzalo Castillo, Vice President of research and development, responsible for the direction of science at 3D pharmacology service provider BIOENSIS for his insights into overcoming the limitations of 2D pharmacology and improving the predictive capabilities of pharmacological assays using both 2D and 3D cell culture approaches.
Can you tell me about BIOENSIS and the technology it’s using in providing 3D cellular pharmacology services?
BIOENSIS is a preclinical contract research organization (CRO) that specializes in the pharmacology of spheroids. The company’s novel 3D drug testing system enables more accurate in vitro to in vivo predictions, preventing costly expenditures in downstream development. Our aim is to harness the power of 3D cellular models and provide better, more predictive pharmacology than current in vitro methods. We utilize the power of 3D cell culture in vitro for both on-target and off-target applications.
For on-target activities, the focus of our services has been mainly in oncology. We have a broad panel of 3D-cellular models; tumor-derived cell lines that are routinely tested for our clients using cytotoxicity assays, invasion and migration assays, combination assays, and client specific assays, whom we work with one-on-one to customize for their needs. We have also just introduced our immuno-oncology platform therapeutic antibodies in a 3D micro-tissue. As for off-target activities, we are developing a suite of organotypic models primarily focusing on toxicology.
Among the technologies we use in our 3D models are the Corning® Elplasia® plates and Corning spheroid microplates that feature an Ultra-Low Attachment (ULA) surface — their platform is robust, flexible and scalable, enabling us to provide reliable results in a high-throughput format.
What are the differences between 2D and 3D oncology screening?
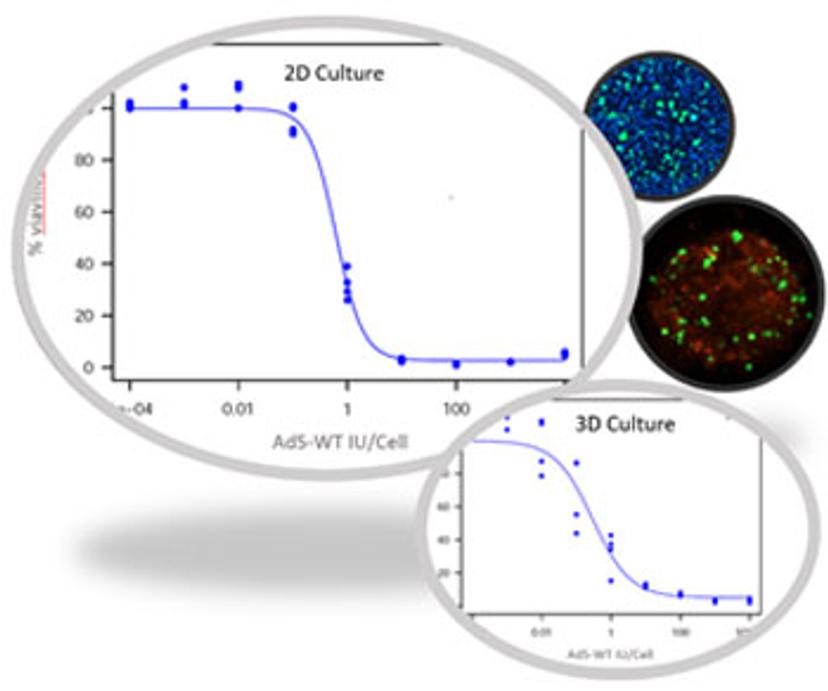
All our models are validated in both 2D and 3D platforms and we routinely run samples in both, depending on our client’s needs. The information obtained in 2D platforms is helpful for discovering the mode of action of the drug. On the other hand, 3D models are helpful in providing information related to drug efficacy. Since 3D models better capture the complexity of a tissue, they are a better predictor of drug responses in vivo. In regard to immuno-oncology, we recently introduced our novel 2D/3D platform that enables efficacy evaluation of therapeutic antibodies for antibody-dependent cell-mediated cytotoxicity (ADCC) and T-cell mediated tumor cell lysis to evaluate the activity of bispecific T-cell engager antibodies (BiTE).
This immune-oncological 2D/3D platform allows for more accurate models to evaluate efficacy that account for cell-cell interaction, metabolic gradients, and antibody diffusion and distribution.
What are the benefits when it comes to 3D systems?
Studies done in cell monolayers may have limited in vitro to in vivo translational value because they do not always capture the known complexity of an organ or tumor microenvironment. In 3D cell cultures, we can account for cell-cell interactions, tumor microenvironments, and formations of metabolic gradients. Another benefit of 3D cell culture, and where 2D cell culture is lacking, is adding the natural complexity of running mixed cell populations to spheroid formation and testing. These factors are vital to understanding drug efficacy and resistance. Spheroidal 3D tissue cultures are one step closer to representing in vivo tumor responses, allowing for greater predictive power in drug candidacy.
What technology or equipment do you use for spheroid growth? Are there difficulties or have you got a tried and tested formula for different cell lines?
In our work, we must be flexible to meet the needs of the client. Truly our specialty is our one-on-one work we do with the client to create the perfect customized assay and in creating 3D models that might mean different equipment, methods, and/or technology for each 3D model. An example is our cell line profiling platform. For this service we routinely evaluate up to 150 tumor cell lines, in both 2D and 3D in parallel, utilizing our automated high-throughput platform. Even though the assays are fully validated, we routinely customize them to meet each client’s needs; through internal R&D and years of experience, we have developed specialized procedures that allow us to quickly and successfully customize each 3D model. We have found that tight microenvironment control leads to successful spheroid formation.
Where do you see the challenges and opportunities for 3D cell culture in this approach in the future?
Building 3D models of organs and diseases can be overwhelming. In the case of 3D tumor models, it involves determining the optimal microenvironment that will allow for the spheroid to form and survive for the time of the experiment. You may also need to reconstruct the heterogeneity of a tumor. This fine-tuning makes every single model a challenge.
We routinely customize our models, all the components that go into the 3D cellular model must be strictly controlled and validated. While customization can be complex, the resulting model will be far more predictive of an in vivo outcome.
The opportunities for 3D cell culture are endless. This is an underutilized market and it is quickly becoming evident that 3D models can better predict in vivo outcomes. This is why we just introduced our immune-oncology platform, including a 2D/3D antibody-dependent cell-mediated cytotoxicity (ADCC) and T-cell cytotoxicity assays that enable efficacy evaluation of therapeutic antibodies in a 3D micro-tissue. In the coming weeks, we will be adding our antibody-dependent cellular phagocytosis (ADCP) testing capability because we believe this is a future direction for our field.
What’s the biggest scientific story in your field right now?
What a great question! I think the biggest scientific story in in vitro right now is the acceptance of 3D models of organs and disease as the leading predictors for in vivo outcomes. The predictive value of 3D models is coming of age in oncology and toxicology, but newer 3D models in regenerative medicine and personalized medicine are on the horizon.
Want to know more?
Discover more research enabled by Corning Life Sciences 3D cell culture technology:


